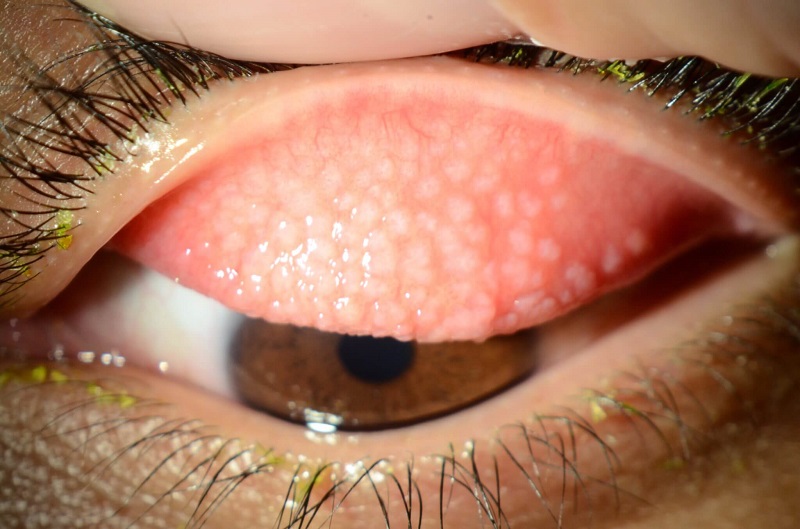
Healthbeauty123.com – Giant Papillary Conjunctivitis (GPC) is an allergic reaction resulting in inflammation of the palpebral conjunctiva, the thin membrane that covers the inside of the eyelids. Optometrists refer to this condition as GPC. GPC is most commonly associated with contact lens use, and is one of the most common side effects of contact lens wear.
Main Causes of Giant Papillary Conjunctivitis
The primary cause of giant papillary conjunctivitis is an allergic reaction to foreign objects, such as pollen, dust, or contact lenses. The eye responds by causing an immunological response. It is not contagious. It is also different from pink eye, which is a bacterial or viral form of conjunctivitis. A physician should consult with a specialist before prescribing contact lens solution.
In addition to hyperemia, patients with GPC may also develop giant papillae. These are patches of active inflammation on the palpebral conjunctiva, with blood vessels in their centers and around their edges. GPC is usually accompanied by other types of papillary conjunctivitis, including vernal keratoconjunctivitis. In addition to Giant Papillary Conjunctivitis, other types of papillary conjunctivitis may also present similar symptoms, including keratoconjunctivitis and scleritis.

Contact lens wearers with GPC may benefit from a contact lens solution that is free of chemicals or preservatives. A patient should replace their contacts as prescribed by their doctor. They should avoid allergen-producing materials and avoid activities that trigger allergic reactions. Most people can wear contacts again after proper treatment. To prevent allergic reactions from developing, individuals should maintain a regular eye exam and avoid using contact lenses for prolonged periods of time.
Occurs Due to Allergic Reaction To Eye Drops
Giant Papillary Conjunctivitis can also result from an allergic reaction to an eye drop. An ophthalmologist may be required to rule out the causes of Giant Papillary Conjunctivitis. If this disease is caused by an allergen, the patient should contact an ophthalmologist for an immediate diagnosis. GPC can also be a symptom of a more serious eye condition called vernal keratoconjunctivitis.
People with Giant Papillary Conjunctivitis commonly wear contact lenses. They are likely to develop this condition if they wear hard or soft lenses. Unlike other forms of conjunctivitis, Giant Papillary Conjunctivitis is triggered by a constant presence of a foreign body in the eyes. This condition can extend to the lower lids and feels like tiny rocks under the eyelids.
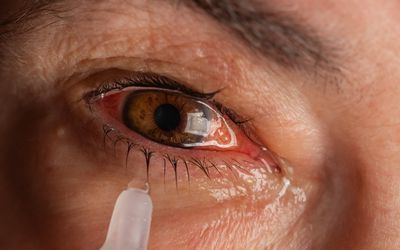
GPC is a chronic inflammatory condition characterized by cellular infiltrates that are characteristic of IgE-mediated atopy. In some patients, an ocular allergy and Giant Papillary Conjunctivitis can occur simultaneously and worsen each other. Inflammatory mediators released during the disease process are released from mast cells, which are the cause of inflammation.
Side Effects of Giant Papillary Conjunctivitis
Giant Papillary Conjunctivitis occurs in both primary and secondary forms. Primary GPC is caused by a foreign object in the eye and occurs in people with seasonal allergies. Secondary GPC develops as the immune response to an allergen begins to wear off. While the primary form lasts forever, a secondary GPC appears later in life. Atopic eczema and contact lenses are the most common causes.
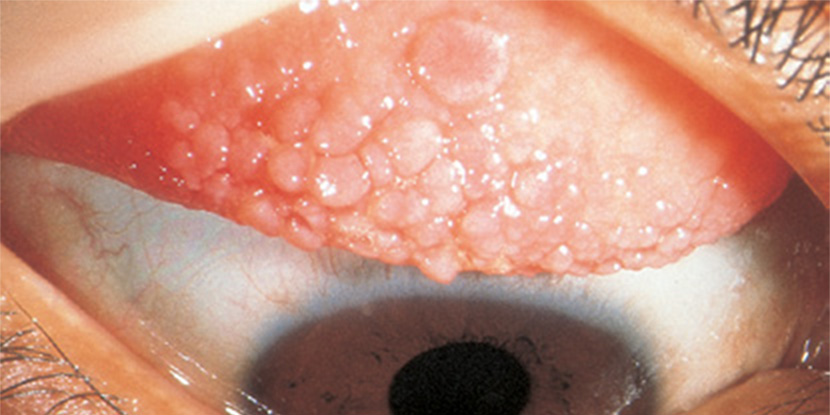
If left untreated, Giant Papillary Conjunctivitis can permanently damage the cornea and eyelid. A doctor can prescribe topical steroids to reduce the symptoms, but these medicines cannot be used for long. Moreover, they can cause unwanted side effects. People who suffer from this condition may have severe irritation, itching, and watering of the eye. Consequently, early treatment is essential. So, it’s very important to seek medical advice if you suspect you have GPC.
Reference: