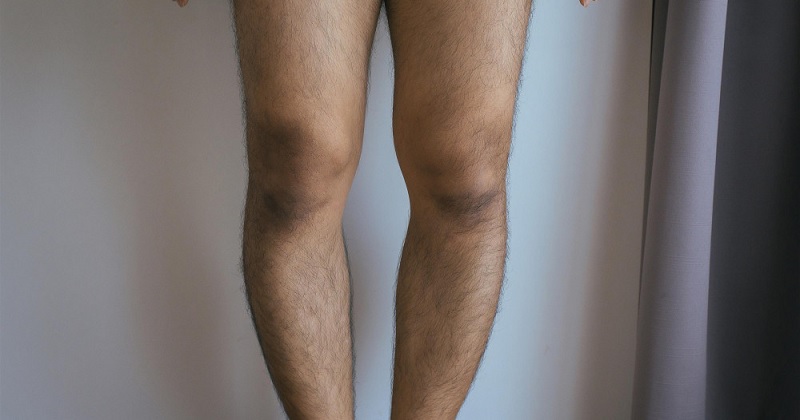
Healthbeauty123.com – A 63-year-old woman presented with severe valgus deformity and a history of congenital hip pain. On x-ray, the femoral condyle was malformed and the bone defects were very severe. According to the Keblish classification, the deformity is classified as severe. The patient was unable to walk normally since childhood. Physical examination revealed slack ligaments around the knee. During flexion and extension, she could only reach an average of 32 degrees.
Genetics Play a Role in the Development of Deformities
While genetics plays a role in the development of the deformity, you can still develop the condition if your parents had it. If your parents had it, you probably have it too. This condition often develops in childhood and can occur in both legs. Fortunately, most knock knees self-correct by the time the child reaches about seven years old. It is important to seek treatment as soon as you notice symptoms.
Surgical treatment for valgus deformity varies. Typically, there are two primary options for TKA: cruciate retaining (CR) and posterior stabilized (PS). CR designs are the more common option. The posterior stabilized design is safer than the CR version, but the PCL tends to contract over time and limit deformity correction. The PS design improves lateralization and patella tracking.
A hinged implant provides optimal stability in severe valgus deformities and multiplanar instability. However, the long stems of these implants are difficult to remove during revisions. Furthermore, there is a risk of loosening and rupture of the prosthesis. If the procedure fails, you may need to undergo a revision to correct the deformity. You may have to wear braces for several weeks or even months to achieve the desired results.
Surgical Procedure for Valgus Knee Deformity
Although a surgical procedure for valgus knee deformity presents challenges, multiple procedures have been described with excellent clinical results. An important aspect of TKA for valgus knee deformity is the stepwise approach to deformity correction. In milder cases, a cruciate-retaining implant can provide adequate stability, whereas a cruciate-sacrificing implant may be required for severe deformities.
In a valgus knee, the surgeon first makes a small cut across the tibial long axis, which decreases the degree of valgus deformity to 3 degrees. He then checks for hypoplasia of the lateral femoral condyle, transepicondylar axis, and balancing in flexion. The tibial cut then restores the joint line and allows a 3-5-deg posterior slope.
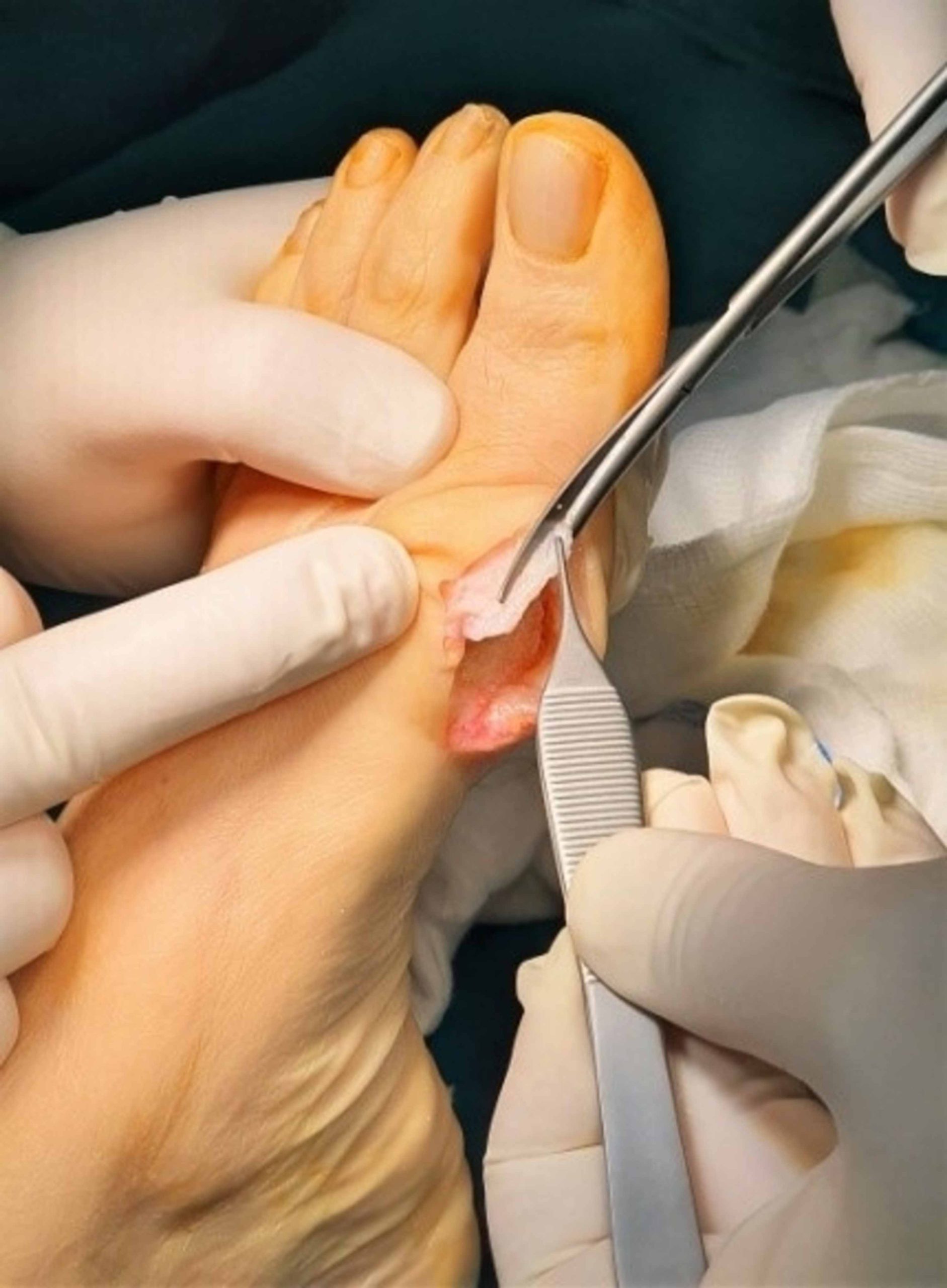
While the treatment for hallux valgus deformity in athletes is no different from that of nonathletes, a surgical correction for this deformity in athletes is not advised, unless it will seriously affect their career. Nevertheless, this treatment option can be effective for a wide variety of individuals, including athletes. But, it is important to remember that there is no definitive cure for this disorder. The goal of this treatment is to prevent further damage and pain.
Surgical Treatment for Valgus Deformity
Surgical treatment for valgus deformity is a surgical procedure for the correction of osteoarthritis in the knee. The surgery involves cutting bone from the distal femur, balancing the medial and lateral ligaments, and restoring the neutral mechanical axis of the patellofemoral joint. Proper balance of the ligaments and the patellofemoral joint is critical for the long-term stability and functional outcome of the implant.

Hallux valgus is a common foot deformity, affecting about 23% of people between the ages of 18 and 65. This condition affects the ability to roll-off, distribute weight, and coordinate gait. It can also cause permanent skin irritation and can even cause the joint capsule and bursa to thicken and become inflamed. The big toe may also bulge against the inside edge of the shoe.
Reference:
Hamer, Andrew J. “Pain in the hip and knee.” BMJ 328.7447 (2004): 1067-1069.