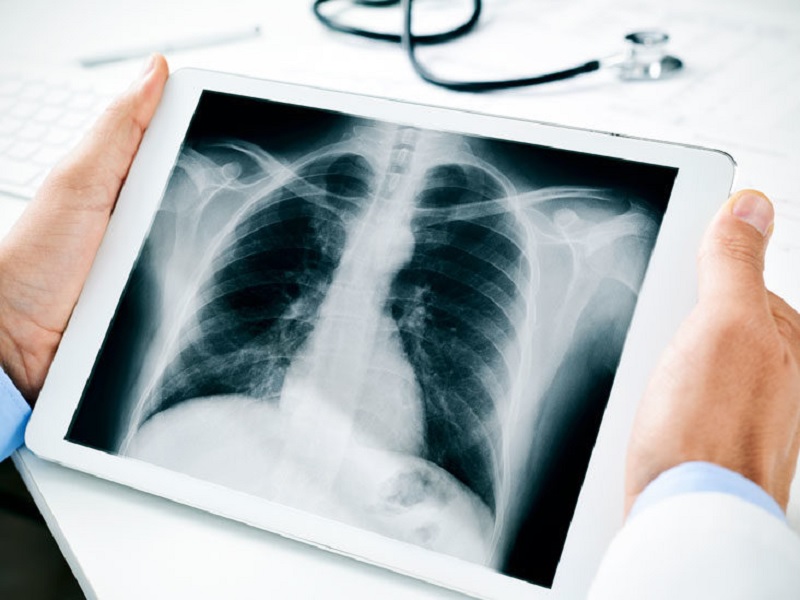
Healthbeauty123.com – The diagnosis of hamartomas is primarily made by wedge or core-needle biopsy, as fine-needle aspirations are nondiagnostic. Pathologic examination revealed single or multiple tumors ranging in size from solid to cystic. Size did not correlate with radiographic findings, though larger lesions were more visible. Surface lesions, on the other hand, remained occult.
Definition of Diagnosis of Hamartoma
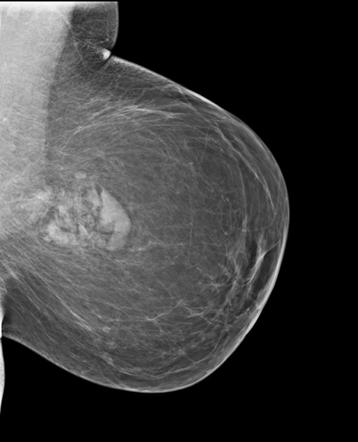
Hamartoma are very rare and slow-growing tumors of the breast. They have the appearance of normal breast tissue and contain fibrocystic foci, although they may be hard to diagnose pathologically. Hamartomas also lack a true capsule and instead have a pseudo capsule that separates them from adjacent breast parenchyma. A typical MRI image of a hamartoma has a diameter of three centimeters or more.
A 42-year-old man presented with left-sided facial numbness. Magnetic resonance imaging showed a solid tumor in the left interpeduncular cistern and a massive arachnoid cyst in the left middle cranial fossa. Histology revealed that the tumor consisted of mainly smooth muscle, but also included squamous epithelium and mucous glands.
Albrecht’s contributions to hamartomata led to little interest in pulmonary hamartomata. However, a search of the literature reveals several articles on pulmonary hamartoma. In fact, this disease is sometimes referred to as chondroma by many clinicians. For example, Hickey and Simpson published a review of 38 cases from the literature and reported two of their own. The tumors that they described were all typical of Albrecht’s criteria. However, Klages also reported cases of chondroma.
Liver Mesenchymal Hamartoma More Visible on MRI
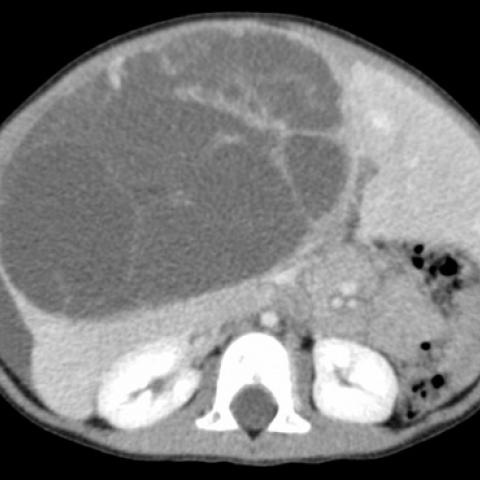
In contrast, liver mesenchymal hamartomas are more visible on MRI and MRCP than other types. Their contrast enhancement differs, but they are hypodense in post-contrast CT and appear hypoechoic on T1-weighted MRI. When the tumors are enlarged, they are mainly cystic and hypodense on post-contrast CT and MRI.
Unlike lung hamartomas, splenic hamartomas are benign tumors that present no symptoms. The frequency of occurrence ranges from 0.014 to 0.13 percent. Often incidental discoveries, splenomas can occur in an otherwise healthy patient. Sometimes, they coexist with hamartomas, such as thrombocytopenia or tuberous sclerosis.
Fibrolipomatous hamartomas are rare and typically arise in the median nerve. They can also occur in the ulnar nerve, lumbar nerve, and sciatic nerve. A computer-based search was conducted for MR images of the musculoskeletal system. The MR images and medical files were then reviewed by two musculoskeletal radiologists. Three consultation cases were also included to further analyze the characteristics of the image.
Hamartomas Can Cause Devastating Epilepsy
Although hamartomas are uncommon, they may cause devastating epilepsy. Their imaging characteristics often make them difficult to differentiate from other developmental tumors. They are often associated with microscopic cortical dysplasia, underscoring their malformative etiology. In most cases, hamartomas can be surgically removed, with seizure free outcomes, although recurrences are also possible.
Visual assessment of macroscopic fat in the lesion is the best method to diagnose pulmonary hamartoma. Pixel analysis and mean attenuation were not helpful for lesional characterization. Combining these two methods improved the specificity to 100%. The results showed that the percentage fat-attenuating pixels in the inner two-thirds of the lesion are useful for diagnosis. The authors describe the clinical and imaging findings of an infant with lingual hamartoma.
The majority of patients with a hamartoma are categorized as solid adenocarcinoma. Their largest diameters ranged from 9.1 to 40.0 mm. The patients who had pulmonary metastasis were classified as a negative group. In order to make the diagnosis, the radiologists evaluated the hamartoma size and location. The radiologists also determined whether the lesions were segmented or calcified.
Reference: